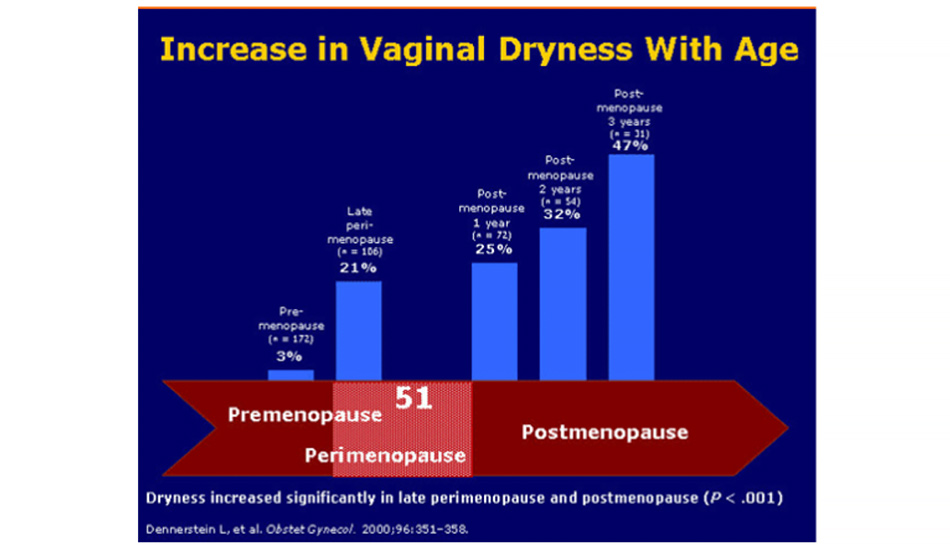
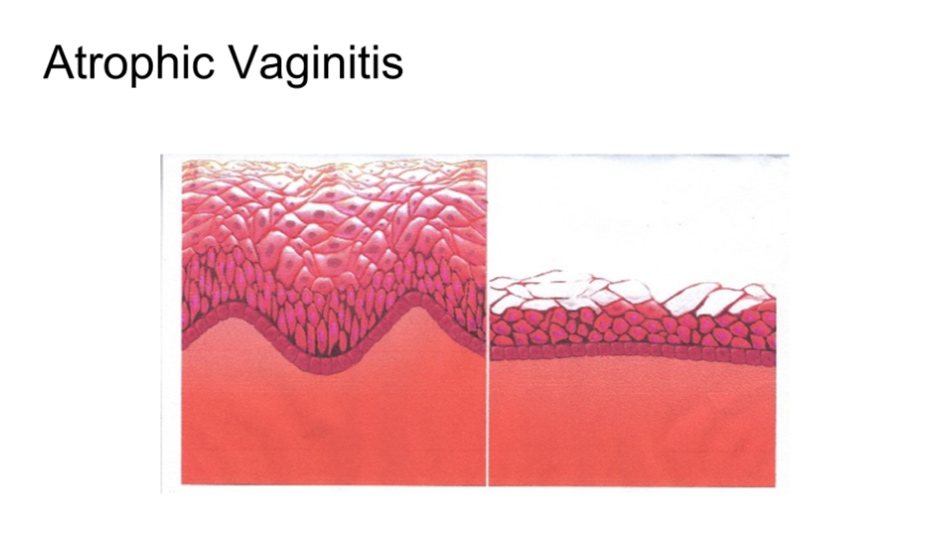
Vaginal atrophy (VA) is also known as vaginal dryness and atrophic vaginitis, and occurs after the menopause. VA can also affect the vulva and can result in vulvovaginitis, and as a result give rise to the Genitourinary syndrome of the menopause.
Vaginal Atrophy occurs as a direct result of oestrogen deficiency. This lack of oestrogen will lead to a reduction in blood follow to the vaginal tissues, and cause: a characteristic thinning of the vaginal mucosa, a loss of collagen tissue, and a reduction in vaginal fluids.
The vagina is a sensitive structure, and needs not only adequate blood flow, but also collagen and a natural release of fluid to maintain its integrity. Collagen will provide elasticity to the vagina and allows the tissues to contract and tighten. Collagen gives the vaginal tissue its elasticity, so that the walls of the vagina can contract and tighten.
The vaginal glands produce a lubricating fluid which maintains vagina’s moisture, and also a low vaginal PH. This not only keeps the vagina clean but prevents infections such as BV and thrush. The fluid also prevents urinary tract infections.
Several over the counter medications including allergy and cold medications, and prescription antidepressants can affect the vaginal mucosa resulting in vaginal dryness.
Vaginal dryness may affect women of any age, but in my experience:
- The majority are Post-menopausal women.
- Women who have had treatment for breast cancer.
- Breast feeding women (again oestrogen is suppressed).
- Women who have undergone a hysterectomy.
- Women who have had treatment with chemotherapy.
Vaginal Atrophy symptoms will include vaginal dryness, vaginal burning, sore sexual intercourse, a loss of the normal vaginal discharge, occasional bacterial vaginosis, labial itching, and a burning pain on passing urine. The loss of the acidic vaginal pH will also lead to frequent urinary tract infections, occasionally urinary incontinence. The loss of the vaginal mucosa will lead to bleeding after intercourse.
- Menopausal women make up 60% of those affected.
- Vaginal Atrophy can result in recurrent UTIs and bacterial soreness.
- Some over the counter preperations can cause vaginal dryness.
- Women who have had breast cancer are also at risk.